 (rollover to compare with normal)
(rollover to compare with normal) |
|
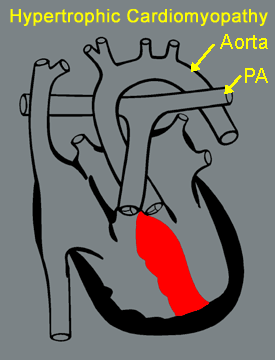
What Are Its Effects?
The thickened ventricular septum may obstruct the outlets to the aorta and/or pulmonary artery (PA), elevating left ventricular pressure and if severe, reducing coronary perfusion. However, there is no obstruction and therefore no murmur in the majority of cases.
Many patients experience no symptoms except during periods of exertion, when chest pain and shortness of breath may occur. Hypertrophic Cardiomyopathy (HCM) may also cause fainting spells, arrhythmia (irregular heart beat), heart failure, or even death. Patients with severe hypertrophic cardiomyopathy are at risk of dying suddenly from abnormal heart rhythms.
HCM may be readily diagnosed through a variety of tests, including electrocardiography (producing an ECG, or electrocardiogram) and echocardiography (producing an echocardiogram). The ECG will show abnormalities in 80-90% of HCM patients. About 25% of patients will develop arrhythmias (e.g. ventricular tachycardia, atrial fibrillation). A heart murmur may be present, characterized by changes in its nature depending on the position of the patient. Typically, the murmur will decrease in intensity as the patient goes from a standing to a squatting posture, and vice versa.
Hypertrophic Cardiomyopathy patients with no left ventricular outflow tract (LVOT) obstruction may have diastolic dysfunction (abnormalities in the interval between heart contractions, when the chambers fill with blood).
It is important to identify those patients who are at risk of sudden death. A history of cardiac arrest, a family history of sudden death from HCM, arrhythmia, recurrent fainting spells (syncope), abnormal vascular function during exercise - all are reasons for caution. Treatments to ward off sudden death involve medication with amiodarone and the implantation of ICDs (implantable cardioverter defibrillators, which will shock the heart to restore normal rhythm if necessary), both of which protect against fatal arrhythmias. |